Deciding on a Patient’s Life in a Democratic Context
Most countries in the wider trans-Atlantic space try to adhere to democratic values, the rule of law and respect for human rights. Regarding the latter, the right to life and the inviolability of human dignity are prominently enshrined in most of their constitutions. They form the very foundation of the moral and ethical core beliefs of the international community of liberal-minded states. As a result, the health care sectors of these countries attempt to cure all patients regardless of their backgrounds or affiliations. Doctors apply state-of-the-art medical treatments to try to cure the most serious of diseases. However, this maxim was challenged when the COVID-19 pandemic hit Europe and North America.
In early 2020, the Western public was not overly concerned about news of the coronavirus. That changed dramatically when COVID-19 began to spread at the end of February that year. The virus was especially virulent in Western Europe. Hot spots were Barcelona, London, Bavaria, northern Italy and the French region of Grand Est. Reports of Lombardian and Alsatian hospitals in distress began appearing in European news outlets. By mid-March, the public was shocked to learn that Italian physicians had too few ventilators to save all COVID-19 patients. Most European hospitals did not have a sufficient number of intensive care units equipped with desperately needed ventilators. Consequently, doctors were forced to decide which patients received which treatments. The Italian Society of Anesthesia, Analgesia, Resuscitation and Intensive Care (Società Italiana di Anestesia, Analgesia, Rianimazione e Terapia Intensiva, or SIAARTI) issued recommendations for doctors on how to deploy scarce resources. Prioritizing medical treatment is called triage. In essence, it can be a life or death decision. With regard to the principles laid out above, triaging patients might be incompatible with the constitutionally safeguarded right to life and its accompanying protection. This article aims to shed light on the question of how democratic states can adhere to their highest constitutional principles while facing a pandemic.
What is Triage?
Under normal conditions, health systems make all resources available to save a patient’s life. However, the very nature of mass accidents, catastrophes, armed conflict, terrorist attacks or pandemics may force the health sector to prioritize its capabilities and capacities according to what is manageable. This is where triage comes into play. The term originates from the French verb trier. It means sort, select or separate. In the medical context, triage is a classification with regard to the urgency and intensity of measures needed to treat a patient. For instance, a lightly wounded patient needs less attention than one who is severely wounded. The situation becomes problematic when a patient has suffered severe injuries that require personnel and equipment that could affect the survival of others. Medical staff must then analyze the probability of a patient’s survival in relation to the available resources to save as many lives as possible.
Triage in History
In Europe, the practice of prioritizing medical treatment dates back to the time of the Napoleonic armies. Military medics based their therapies on a prognosis of the chances of survival of the wounded. Already, at the turn of the 18th and 19th centuries, tags were used to indicate each soldier’s diagnosis. During World War I, the triage and tag procedure became more sophisticated. Throughout the 19th and 20th centuries, purely medical considerations were coupled with the overall aims of the conflict parties. This led to more categorizations of treatment priorities. For instance, soldiers enjoyed priority over civilians and one’s own soldiers enjoyed priority over the enemy’s injured. The triage and tag system developed further during the Cold War era. Under the assumption that a nuclear war would extremely limit the health sector’s capacity to treat the injured, medical staff were prepared to apply a rigorous prognosis to those who could possibly survive radioactive contamination.

Today, most health sectors have developed an advanced system of tags for medical first responders in case of a mass casualty incident. The triage tags are meant to enable personnel to effectively and efficiently distribute limited resources and provide the necessary immediate care for victims until additional help can arrive on the scene. The tags are usually color-coded. Black stands for “expectant,” meaning the injured person is expected to die. In such a case, patients only receive pain-relieving medication. Red is for patients who have suffered life-threatening injuries and signals the need for immediate treatment. A yellow tag means that the person has non-life-threatening injuries but that urgent help is required. Green labels indicate individuals with minor injuries. Most modern ambulance vehicles and mobile intensive care units are equipped with a stack of triage tags to prioritize the injured for subsequent medical transport and treatment in the case of a mass casualty event.
Narrowly understood, triage is a toolkit designed to be medically useful in the event of a mass casualty incident or disaster. Its underlying philosophy is called “utilitarianism.” Utilitarianism attempts to provide the most benefits to the highest number of people possible. As a normative ethical theory, it intends to maximize well-being for all affected people. It dates back to philosophers such as David Hume and John Stuart Mill in the 18th and 19th centuries. However, a purely utilitarian approach to justify medical triage might not stand a legal assessment. Emphasizing the state’s responsibility to protect the right to life, lawyers might look at triage decisions differently.
Legal Considerations
The aforementioned SIAARTI guidelines basically mirror the triage classifications. Faced with a limited number of ventilators and trained staff to treat all those infected with COVID-19, the guidelines made three recommendations for Italian clinicians. First, priority should be given to those who have a greater likelihood of survival. Second, focus on patients who have more potential years of life. Consequently, patients with underlying conditions and elderly persons who are deemed to stand less of a chance of surviving the coronavirus may not be treated in favor of healthier and/or younger patients whose chances of recovery are higher. Lastly, clinics are advised to make maximum use of the scarce resources for as many patients as possible. Some doctors voiced dismay at being asked to apply these recommendations.
The situation in Germany was in some ways similar. In March 2020, virologists and epidemiologists calculated that approximately 40,000 intensive care units would be needed to cope with the expected number of patients throughout the Federal Republic. At the time, hospitals had roughly 10,000 ventilators on hand. The Deutsche Interdisziplinäre Vereinigung für Intensiv- und Notfallmedizin (DIVI), a German association equivalent to the Italian SIAARTI, also issued a set of recommendations. They are comparable in principle, but details differ. For instance, the DIVI guidance does not contain a similar recommendation to base decisions on the assumed life expectancy of patients. It also forbids prioritization based solely on age or social criteria. The DIVI does, however, recommend prioritizing patients based on higher survival probability and that medical personnel constantly assess all patients in a hospital, including those not infected by the coronavirus. The assessment has to take into account the prognosis of all patients regardless of their disease. Hence, newly arrived patients with promising prognoses might mean patients in need of ventilators are denied them in favor of the newcomers.
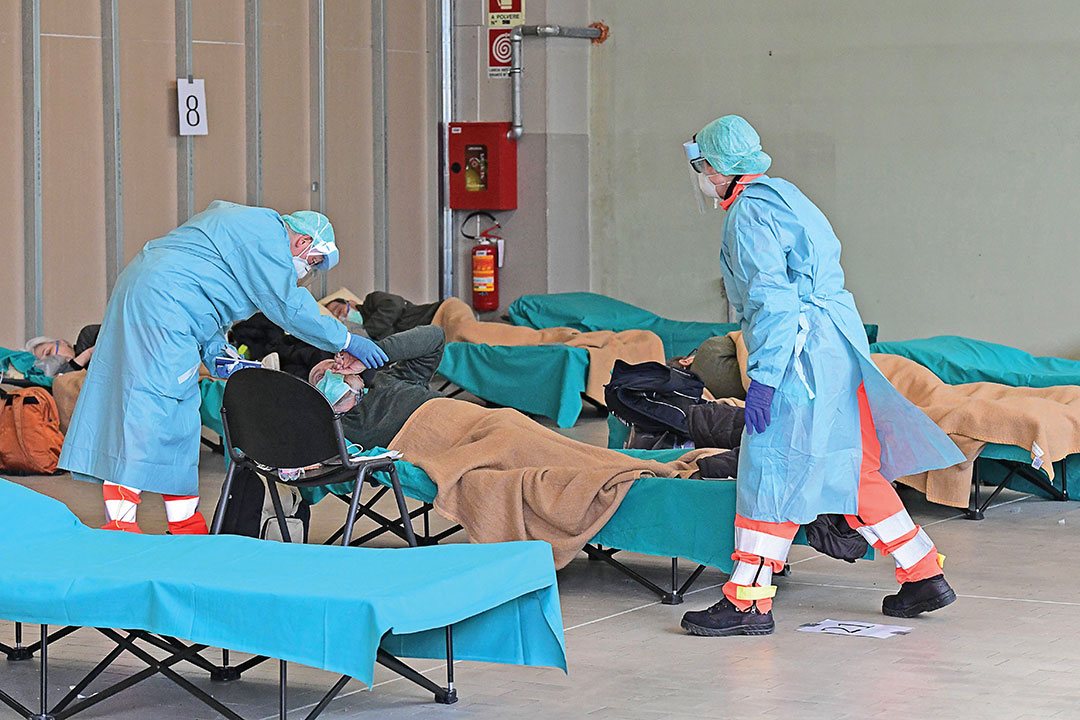
The desperate situation in spring 2020 and the DIVI recommendations caused a discussion among the legal and philosophical communities on how triage decisions could be made in accordance with the law. At first glance, a doctor’s decision to refuse or abort a treatment might constitute a crime under the German Criminal Code; that would be Section 212 applying to homicide/manslaughter: “Whoever kills a person … incurs a penalty of imprisonment for a term of at least five years.”
In a triage scenario, criminal lawyers already differentiate between a doctor’s refusal to treat a patient who is likely to die (omission) and a physician’s decision to shut down a ventilator when the patient is expected to die soon (commission). While omission does not necessarily lead to criminal liability, because there is no duty to save a life, active interference might be a punishable offense. Still, that does not determine whether such an action might be justified. Being mindful that a clinician could remove the ventilator from a dying patient to use it for another with better chances of survival, a judge might apply Section 34 of the Criminal Code: “Whoever, when faced with a present danger to life, limb, liberty, honor, property or another legal interest which cannot otherwise be averted, commits an act to avert the danger from themselves or another is not deemed to act unlawfully if, upon weighing the conflicting interests, in particular the affected legal interests and the degree of the danger facing them, the protected interest substantially outweighs the one interfered with.”
However, this only applies to the extent that the act committed is an adequate means to avert the danger. The problem is that the German Federal Constitutional Court decided in 2006 that sacrificing innocent lives in favor of another group violates the unconditionally protected human dignity principle enshrined in Article 1 of the German Basic Law.
The legal academic community also elaborated on the question of whether there is a different criminal liability for doctors in cases of ex-post triage or ex-ante triage decisions. The term ex-post triage describes the above-mentioned situation when a doctor switches off the ventilator in favor of an incoming patient with a better prognosis. Ex-ante triage describes when a doctor has to decide which of two patients gets the one respirator, according to the predicted chances for recovery. Some scholars acknowledge that, faced with an insurmountable clash of medical, ethical, legal and moral obligations, this is a dilemma for the physician.
Other legal scholars support recognition of a so-called supra-judicial justification. They recommend applying mutatis mutandis Section 35 of the German Criminal Code, commonly referred to as the necessity defense: “Whoever, when faced with a present danger to life, limb or liberty which cannot otherwise be averted, commits an unlawful act to avert the danger from themselves, a relative or close person acts without guilt.” Another school of thought claims that a patient whose chances of survival are low would hypothetically be willing to interrupt his treatment to save a fellow human being with better chances of survival. Finally, a number of legal scholars simply suggest accepting the fact that triage constitutes a criminal liability for a clinician.
The debate intensifies and slides into the discipline of philosophy when two patients who have the same health prognosis compete for a respirator. This could mean that medical personnel apply their own personal moral beliefs. Is a younger life worth more than an older one? Should a pregnant woman be given priority over a male? Is the patient a father or a single man? Some suggest that the physician should base his decision on the so-called fair innings argument, which justifies refusal to treat an elderly patient in favor of a younger one based on the perception that the death of an older person is unfortunate but the death of a younger person is tragic.

In “Corona Triage – A Commentary on the Triage Recommendations by Italian SIAARTI Medicals Regarding the Corona Crisis” in the Verfassungsblog, philosophy Professor Weyma Lübbe argues against the utilitarian justification of maximizing the number of years of life saved. She believes that this principle leads to inhumane consequences and introduced the following scenario: According to this principle, a 60-year-old woman would have to be denied treatment with a ventilator in favor of a 20-year-old man, even if she could very likely (70%) be saved by the treatment. Without the treatment she would die. The 20-year-old would probably survive even without treatment (70%), but his probability of survival could be improved to almost 100% with the treatment. This calculation shows that in such a case, more years of life could probably be gained if the 20-year-old was ventilated, not the 60-year-old. Lübbe continues: “Rights are non-aggregatory. In times of shortage, they do not need to be maximized, but rather specified in a just manner.”
Admittedly, none of these approaches seems to be fully satisfying. Neither the German nor the Italian recommendations, nor the respective academic debates offer a definitive course of action to avoid criminal liability. A doctor’s decision on a human’s fate in a triage scenario seems to lie “beyond justice.”
The ‘Beyond Justice’ Dilemma
Some staged propaganda operations by Eastern Hemisphere powers have insinuated that the Western model of rule-based democracy is failing to cope with the pandemic. Does the discussion on legal and ethical dilemmas mean that democracies will fail due to their own norms and principles when challenged by COVID-19? A brief historical review reveals that the current search to find an adequate response to the legal and ethical dilemmas involved has been ongoing for more than 2,000 years.
In the 2nd century B.C., the Greek philosopher Carneades came up with an ethical-legal thought experiment: Two shipwrecked sailors find a plank in the sea that can only carry one person. One sailor swims faster and gets to the plank first. The other sailor makes it to the plank, but since he is stronger, he pushes the first sailor off. The sailor who was thrown off the plank drowns and the sailor who successfully fought for the plank is later rescued. Carneades and his followers pondered whether the surviving sailor could be tried for homicide or murder.
The “Plank of Carneades” was later debated by the ancient Roman philosopher Cicero in the 1st century B.C. Cicero favored the survival of the person who could make credible claims to contribute to society. Immanuel Kant also revisited the scenario in the 18th century and argued that the state might not be able to punish the surviving sailor, but he may nevertheless be culpable. In any case, the Prussian enlightenment philosopher refused to apply the necessitas non habet legem (“necessity has no law”) maxim to Carneades’ scenario. If the “Plank of Carneades” case were to be tried before a German criminal court today, the surviving sailor would most probably be found guilty of having committed a crime according to Section 212. However, his attack on the sailor who got to the plank first would be excused under the above-cited necessity-defense provision according to Section 35 of the Criminal Code.
Another scenario that demonstrates the shortcomings of law in relation to moral and ethical challenges is a case modeled on Gerhart Hauptmann’s late 19th century novel Bahnwärter Thiel (Signalman Thiel). The legal scenario is based on a signalman watching as his son crosses train tracks while a train full of passengers approaches. If the signalman flips the switch, diverting the train, it will crash causing numerous casualties. If he does not, the train will hit his child. While this scenario was actively debated in German law schools, an English court had to decide a case of morality, ethics and legality. The 1884 case of R v. Dudley and Stephens dealt with three shipwrecked sailors, two of whom survived. The question for the court was if they were guilty of homicide because they killed and ate their shipmate. The judges found that there could be no necessity defense based on legal precedent or because of ethics and morality. The judges believed that preserving “one’s life is generally speaking a duty, but it may be the plainest and the highest duty to sacrifice it.” They also questioned the self-given power of the two surviving sailors to decide whether the third person should be killed for the sake of their survival. The accused were sentenced to death, but later pardoned and released.
Turning to modern times, a 2006 case at the German Federal Constitutional Court needs to be revisited. In response to 9/11, the parliament enacted the German Aviation Security Act in early 2005. This law allowed the German Armed Forces to down a commercial airliner if it was apparent that the plane was being used as a weapon by hijackers. The former president of the Federal Republic, Horst Köhler, raised doubts about the act’s legality at the time. Although he ultimately signed the act, he recommended that the Constitutional Court in Karlsruhe check its compliance with German constitutional principles, including the inviolability of human dignity principle and the right to life.
Ultimately, two former interior ministers of German federal states challenged the Aviation Security Act. The pro-Aviation Security Act camp argued that a plane with 100 passengers must be shot down to save the lives of 80,000 people if the hijackers intended to direct the plane into a sold-out football stadium. The opposing side argued that the lives of the passengers in the plane were just as valuable as those of the football spectators. The judges basically decided in favor of the latter view. Weighing one life against another is unconstitutional regardless of any qualitative or quantitative considerations. The ruling meant that the state would not decide who should survive; in this case, a smaller group of passengers or a larger crowd of football spectators. Interestingly, two federal ministers of defense in two different coalition governments during this time period declared they would have ordered shooting down a hijacked plane to prevent more casualties on the ground. However, they both stressed that they were mindful of the dilemma and promised they would have stepped down from their positions the very same day.
Summary
No reasoning could produce a satisfactory course of action with regard to the legal dilemma encountered when human lives stand in the balance. In this regard, authoritarian regimes have an advantage when dealing with pandemics. They have no need to consider ethical and legal values such as the inviolability of human dignity or the right to life. Thus, rule-of-law-abiding democracies may lag behind those that abuse pandemics to showcase their models of single-power rule. There is a more than 2,000-year history of Western philosophers and jurists struggling to come up with benchmarks for when one life might trump another.
Humanities scholars and lawyers have also attempted to define when the person making a life-terminating decision is criminally liable and when such an action might be justified, excused or understood as “beyond justice.” Rigid authoritarian regimes can simply prioritize available medical assets for the survival of loyal cadres, essential functionaries, powerful family clans, wealthy oligarchs, or along ethnic, religious or other group affiliations. In addition, access to legal remedies is often limited. As a result, authoritarian regimes need not fear that relatives will attempt to seek criminal justice on behalf of deceased family members.
In Europe, the panic to not overburden health systems and thereby cause more deaths in hospitals led to Europe-wide shutdowns of public life. Governments introduced harsh restrictions to enforce social distancing. Schools, airports, restaurants, bars, gyms, retail shops and some administrative inner-state borders were closed. Visits to hospitals and nursing homes were prohibited. Office workers were encouraged to telework from their homes. By the end of March 2020, many European cities had turned into ghost towns, but the curve of COVID-19 infections did flatten and reports of physicians triaging patients disappeared. The subsequent months were used to identify available treatment capacities in other European countries and to outfit the health sector with additional intensive care units.
Germany, for instance, was able to reach the desired 40,000 beds with ventilator machines. Certainly, other aspects of the COVID-19 pandemic, such as the economic impact of the shutdown, mattered more in the public debate. Yet the enormous investments in Germany’s critical health sector helped the Federal Republic avoid triage decisions. So far, the judicial impact of medical decisions has not been tested. While this article was being written, there was no case filed at Europe’s highest court dealing with human rights violations. Legally, it would be possible to turn to the Strasbourg-based European Court of Human Rights. For instance, dependents of a deceased patient may turn against a member state refusing to try a clinician for a particular triage decision. The court could then indirectly assess whether Article 1 (The High Contracting Parties shall secure to everyone within their jurisdiction the rights and freedoms defined in Section I of this Convention) and/or Article 2 (Everyone’s right to life shall be protected by law) of the European Convention on Human Rights were violated.
Outlook
Recommendations like the ones from SIAARTI or DIVI still circulate in European hospitals. At this stage, they are a medical basis upon which a doctor might make a triage decision. Henceforth, utilitarianism still shapes the medical decision-making process, taking into consideration a higher probability of survival and the use of limited resources to save as many lives as possible. In parallel, legal and philosophy scholars will continue to discuss whether the suggested courses of action could constitute a criminal liability.
The SIAARTI or DIVI guidelines are what they are: sets of recommendations by associations of medical experts. They are not law. In addition, these expert associations are not representing any governmental authority that could be held responsible. From a lawyer’s view, it seems desirable that if basic rights are essentially to be interfered with that these encroachments be based on a solid law. Triage decisions do constitute interference with regard to an essential right, which is the right to life.
While it was understandable that intensive care experts felt the need to draft guidelines for their doctors during the peak of the pandemic, it would also appear necessary to exclude them from criminal liability. For practical and obvious reasons, society should expect that the health sector is doing its utmost to cure patients, especially in cases such as the current COVID-19 pandemic. Doctors should not also have to fear being prosecuted for homicide.
Finally, the triage dilemma of trying to cure the maximum number of patients with limited resources is linked to a democratic society’s expectations in terms of foreseeability. Going forward, it will be imperative that the law describes the conditions under which triage can occur. For legislators, this means revisiting a centuries-old debate about this moral, ethical and legal dilemma. Nevertheless, clarifying how the very fundamental right to life and inviolability of human dignity can be maintained while countering the virus is worth the effort. In view of the ongoing global competition regarding governance models, triage laws would be a written statement on how patients are to be cured in an ethical and nondiscriminatory manner.


Comments are closed.